The UEAHSCP Medicines Optimisation Group East Anglia (MOGEA) has been supported by NIHR CLAHRC Eastern to develop an approach to opioid tapering.
We have combined research evidence with experiences of health organisations and individual practitioners and developed a service specification that can be translated across regions.
Project background
Evidence for the long-term benefits of opioids to manage chronic non-cancer pain (CNCP) is limited and evidence for harm is growing.(1) Reducing opioid prescribing is an NHS Improvement goal (2) and MOGEA (NNUH, JPUH, QEHKL, WSFT, NCH&C, Ipswich, NSFT) have unanimously identified this as a regional priority. A 2018 BMJ review reported the quality of published evidence for opioid deprescribing interventions to be low, and no evidence for their efficacy or safety. The BMJ review recommendations on opioid reduction were therefore based on expert opinion rather than empirical evidence of benefit. The continuing rise in opioid prescribing for CNCP demonstrates the need for more research which can be widely implemented.(3, 4)
The result of this focus on reducing CNCP prescribing is numerous local and national activities each with varying levels of success. We have undertaken a realist review which offers a structured approach to capturing the details of these local and national activities in order that we may learn from the existing research literature and the practice environment. A realist review aims to understand what elements of these attempts to reduce CNCP prescribing are effective, for whom, under which circumstances and how. Examples of circumstances include the relationships and attitudes of individuals providing the service, and environment in which the service is delivered. Through the realist review we have therefore been able to identify the key service elements and conducive circumstances and design an opioid deprescribing intervention with effective components that best fit the circumstances that can be feasibly replicated.
To identify the mechanisms by which opioid deprescribing interventions are believed to result in their intended outcomes.
To explore the contexts which determine whether the different mechanisms produce intended outcomes.
To identify and share materials to support opioid deprescribing.
To develop an intervention specification for opioid deprescribing suitable for feasibility testing.
Project Process
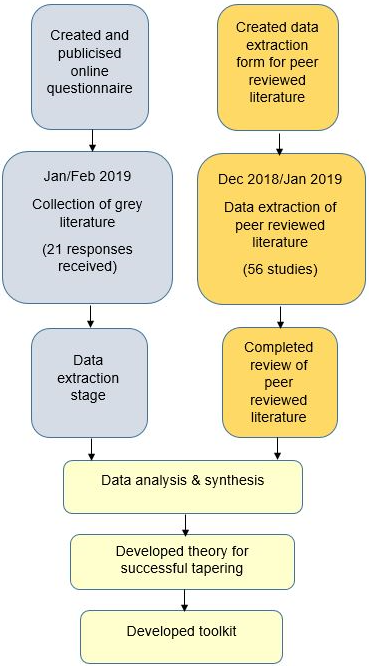
Project results
Following analysis of the evidence we have developed the following theory about what elements are essential for the successful tapering of opioids:

Toolkit
Documents referred to in the toolkit:
2017 Canadian Guideline for Opioids for Chronic Non-Cancer Pain
CDC Pocket Guide: Tapering Opioids for Chronic Pain
Dorset Opioid Prescribing for Chronic Pain: Resource Pack
NPS Medicinewise Recommendations for deprescribing or tapering opioids
Prescribing Incentive Scheme (PIS) 2017-18 Medicines Management Team
Supporting documents
Supplementary file 1 - Initial Programme Theories
Supplementary file 2 - Development of Programme Theories
Supplementary file 3 - Mid Range Theory
Online survey form - Tackling Opioid Use in Non-Cancer Chronic Pain
For further information about the project please contact the project lead - Debi Bhattacharya: d.bhattacharya@uea.ac.uk
Our Research Team
Debi Bhattacharya
Hattie Whiteside
Emma Tang
Kumud Kantilal
Yoon Loke
Caroline Hill
Bethany Atkins
This research is registered with PROSPERO - registration number CRD42019121838
References
Manchikanti L, Kaye AM, Knezevic NN, McAnally H, Slavin K, Trescot AM, et al.
Responsible, Safe, and Effective Prescription of Opioids for Chronic Non-Cancer Pain: American Society of Interventional Pain Physicians (ASIPP) Guidelines.
Pain physician. 2017;20(2s):S3-s92.
Faye’s story: good practice when prescribing opioids for chronic pain: NHS South region South West; 2017 [Available here]
Berna C, Kulich RJ, Rathmell JP.
Tapering Long-term Opioid Therapy in Chronic Noncancer Pain: Evidence and Recommendations for Everyday Practice.
Mayo Clinic proceedings. 2015;90(6):828-42.
Sandhu H, Underwood M, Furlan A, Noyes J, Eldabe S.
What interventions are effective to taper opioids in patients with chronic pain?
BMJ. 2018;362.

:focus(1360x649:1361x650))